Disc Herniations: Effectiveness and Safety of Spinal Manipulation
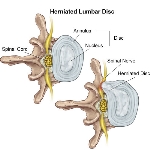
The management of disc herniations, both in the neck and low-back, is controversial. Surgical care is generally reserved for patients with chronic, debilitating leg dominant pain with MRI confirmation of the disc herniation impinging on the affected nerve. Even in these cases a trial of conservative care is warranted prior to opting for surgery.
So what are the conservative care options for a patient with a disc herniation? Medical management may include prescription strength anti-inflammatories, epidural nerve root injections or a watch and wait approach. Manual therapists may recommend nerve flossing, traction, joint mobilisations and/or exercises (ie. McKenzie exercises, core stability exercises or general movement based recommendations). Other general advice such as to keep moving, avoid sitting and whether or not to use ice is often utilized as well.
What about spinal manipulation or adjustments for a patient with a disc herniation? Are they a safe and effective treatment option? Several recent Swiss based studies from the University of Zurich have given us the best evidence to date to answer these questions.
Is spinal manipulation an effective treatment option for patients with a disc herniation?
A 2014 study on 148 patients with a symptomatic lumbar (low back) disc herniation with leg pain (sciatica) all had a MRI confirmed disc herniation at the corresponding spinal segment. The MRI location of the herniation and the physical examination findings were used to select the type of spinal manipulation procedure used. It is important to note that severe herniations (including extrusions and sequestrations) were not excluded from this study. The results concluded that both acute and chronic disc herniation patients on average improved quickly and remained improved up to 1 year. More specifically 70% of patients reported they felt better or much better after 2 weeks and 90% felt better or much better at 3 months.
A similar study was also performed on cervical spine (neck) disc herniation patients with arm pain. The findings largely echoed those of the low back study noting patients with cervical disc herniations with radiculopathy (arm pain) treated with spinal manipulation reported high levels of clinically relevant improvements. 69% of patients reported clinically relevant improvement at 1 month and 85% reported the same at 3 months.
How does spinal manipulation effectiveness compare to image guided nerve root injections?
Therapeutic nerve root injections are an established medical treatment for symptomatic disc herniations. Another study from the same Swiss research group found that both groups (spinal manipulation and nerve root injection) of patients with symptomatic lumbar disc herniations improved at 1 month. However, a higher proportion of patients treated with spinal manipulation reported clinically relevant improvement compared to the nerve root injection group. A 2nd similar study by the same group (accepted for publication in JMPT) for cervical disc herniation patients showed even more significant results in favour of spinal manipulation with cervical disc herniation patients more likely to report relevant improvement versus the nerve root injection group.
Is spinal manipulation a safe treatment option for patients with a disc herniation?
In the above noted studies worsening was reported 0%-2.8% of disc herniation patients treated with spinal manipulation. In comparison, 4-6% of the case matched patients treated with image guided nerve root injections reported worsening. No adverse events from spinal manipulation were reported in either trial. In addition there are several researchers at the University of Toronto (Drs. Hincapie and Cote) who are continuing to study the safety of spinal manipulation for disc herniations; and their work to date also supports the conclusion that spinal manipulation is a safe treatment option for disc herniations.
In summary:
- No intervention is completely risk free. However, spinal manipulation is a safe and highly effective treatment option for patients with cervical (neck) and lumbar (low back) disc herniations (for all types and locations of herniations found on MRI).
- Approximately 70% of patients will report feeling better or much better in 2-4 weeks after initiating spinal manipulation treatment.
- Clinical benefits of spinal manipulation are as good (or slightly better) compared to image guided nerve root injections in the management of disc herniations (with corresponding leg or arm pain)
Special thank you to Professor Kim Humphreys who presented the above information at the 2016 CMCC Research Symposium.
